Discover Cupping Therapy Benefits for Detox & Relief
Cupping's Detox & Lymph Drainage at Peaceful Warriors Wellness Center
Health Benefits of Cupping Therapy
| Benefit | Description | Evidence Level |
|---|---|---|
| Pain Relief | Cupping therapy can effectively reduce chronic pain by improving blood circulation and relaxing muscle tension. | Moderate (clinical studies) |
| Muscle Recovery | Athletes often use cupping to expedite recovery from intense workouts by promoting lymphatic drainage and reducing inflammation. | Moderate (anecdotal evidence) |
| Detoxification | The suction created by the cups helps to draw out toxins and impurities from the body, supporting the lymphatic system. | Limited (emerging research) |
Modern Applications
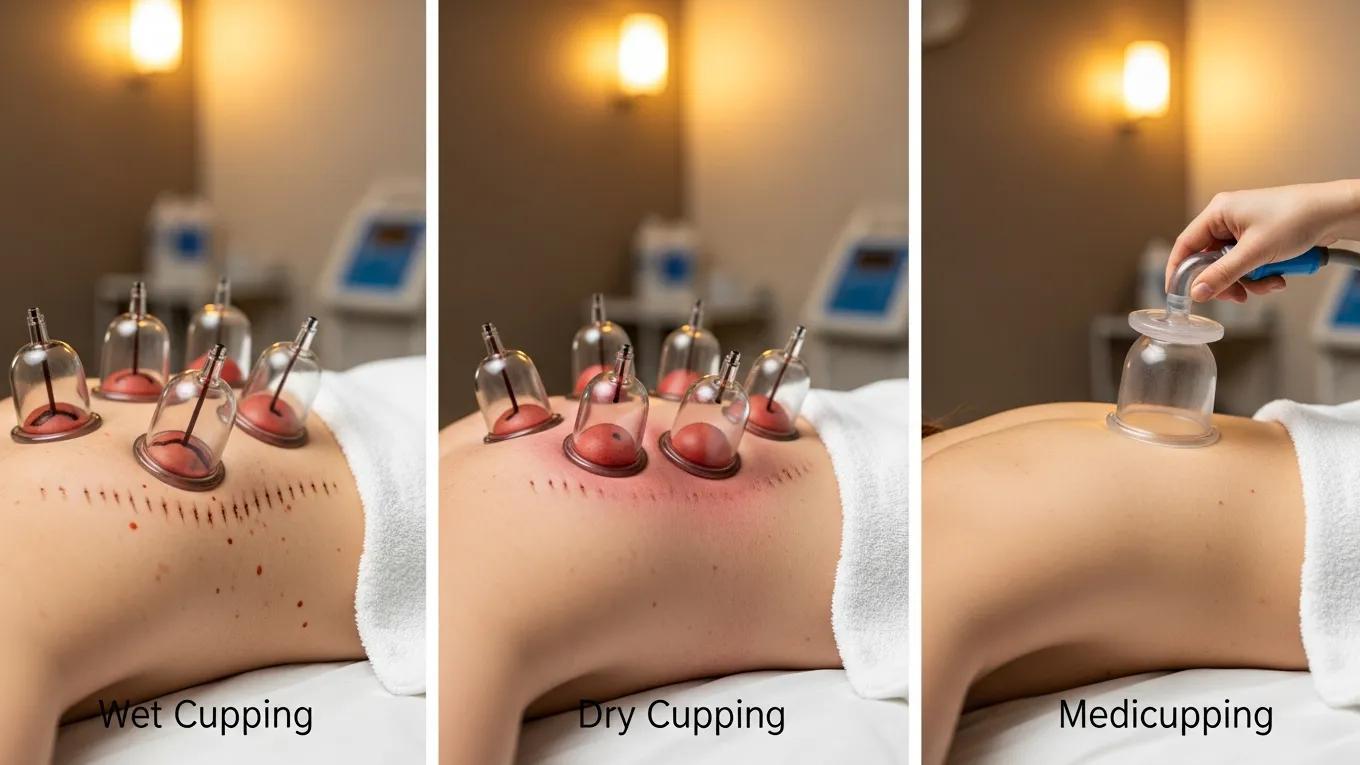
Types of Cupping Techniques
- Dry Cupping: Involves placing cups on the skin without any incisions, primarily for pain relief and muscle relaxation.
- Wet Cupping: Involves making small incisions in the skin before applying cups to draw out blood; often used for detoxification.
- Medicupping: Uses a mechanical pump to create suction, allowing for more controlled pressure and cup movement.